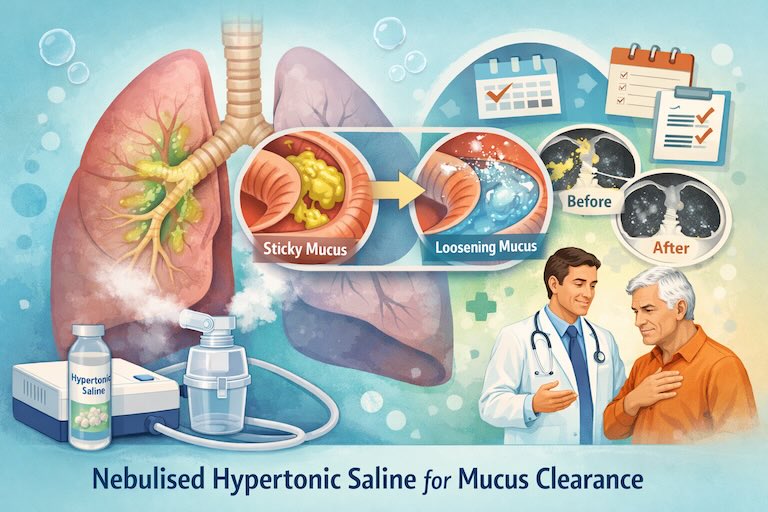
Nebulised hypertonic saline has had a setback. In the 2025 CLEAR trial, adding 6% hypertonic saline to standard care in adults with non-cystic fibrosis bronchiectasis did not significantly reduce flare-ups over 52 weeks compared with no hypertonic saline. The mean number of exacerbations was 0.76 in the hypertonic saline group versus 0.98 in the no-hypertonic-saline group. This difference did not reach statistical significance.
Randomised controlled trials are the best way to test whether a treatment works on average. But “did not help the average patient in this trial” is not the same as “will not help any patient in clinic”. That distinction is important for people living with thick, sticky sputum every day.
Dr Ricardo José still considers nebulised hypertonic saline a useful tool for selected patients, particularly when mucus remains very viscous, difficult to clear, and imaging shows mucus impaction despite properly optimised airway clearance. In his broader bronchiectasis guidance, he consistently emphasises airway clearance as the foundation of treatment and recommends adding hypertonic saline when mucus remains thick, because it draws water into the mucus and helps move it.
What nebulised hypertonic saline actually does
Hypertonic saline is a salty mist breathed in through a nebuliser. Because it is saltier than normal body fluids, it pulls water into the airway surface. In plain English, it helps rehydrate dried-out mucus so it becomes less sticky and easier to cough up.
This is why many clinicians do not think about hypertonic saline mainly as a “flare-up prevention medication”, but as a mucus-mobility aid. If the main day-to-day problem is stubborn sputum that will not move, a treatment that improves mucus clearance can still matter, even if a large trial did not show a clear reduction in annual exacerbation counts.
Earlier smaller studies found better sputum weight, easier expectoration, lower sputum viscosity, and in some trials better lung function or quality-of-life measures, although the overall evidence base has been mixed and small.
Why the CLEAR trial was negative
The CLEAR trial was well designed in many respects and deserves respect. It recruited 288 adults across 20 UK hospitals and looked at a hard clinical outcome: pulmonary exacerbations over 52 weeks. But it tested whether hypertonic saline helped the overall trial population, not whether it helped the subgroup with the stickiest, hardest-to-clear mucus.
This is the first big issue. The trial included adults who produced daily sputum, but it did not require a minimum sputum volume and did not require difficulty clearing sputum for entry.
The investigators openly acknowledged this. They wrote that they did not include criteria based on sputum amount or trouble clearing it, and therefore the results in those specific subgroups remain unknown.
That is easy to understand with a simple example. Imagine testing a strong painkiller in a group that includes many people with only mild pain. The average result may look disappointing, even though the medicine might help the smaller group with severe pain. The same logic may apply here. If hypertonic saline is most useful in people with very tenacious mucus, then enrolling a broader group can dilute that benefit.
The main problem: the trial may have asked the wrong question for the wrong patient
For many patients, the key question is simple: “Will this help me clear the mucus sitting in my lungs today?” They do not usually ask whether a treatment will reduce their annual flare-up count by a statistically significant amount. The CLEAR trial measured flare-ups over one year as its main outcome. That is an important measure. However, it is not the same as looking at immediate mucus clearance, sputum thickness, or whether mucus plugs remain visible on scans.
So the trial really answered this question: “Should hypertonic saline be added routinely for a broad bronchiectasis population to reduce exacerbations?” It did not fully answer this narrower question: “Should a specialist try hypertonic saline in a patient with optimised airway clearance who still has thick, impacted mucus?” .
Other weaknesses worth understanding
Another issue is airway clearance technique itself. Everyone in CLEAR received standard care, including airway clearance. Patients without a routine were taught active cycle of breathing techniques, and all were given an action plan. That is good care, but the trial did not assess airway clearance competency. In other words, the researchers do not know how well patients were actually doing the physio side of treatment. The authors specifically listed this as a limitation.
Why does that matter? Because hypertonic saline is not meant to work alone. It is commonly used before airway clearance to make the mucus easier to move. If someone is not doing the breathing technique effectively, the saline may not show its full benefit. It is a bit like loosening mud with water but never using the shovel properly.
Adherence is another practical problem. The trial authors reported that adherence to oral carbocisteine was higher than adherence to nebulised hypertonic saline. That reflects real life. Nebulisers take time, add treatment burden, and some people find saline irritating. If patients do not use it regularly enough, the measured benefit in a trial will shrink.
The researchers did not power the study to assess differences between subgroups. So even if a subgroup of patients with very thick sputum truly benefits, the CLEAR study could not reliably detect that effect.
There were also differences in dropout numbers between groups, the trial took place only in the UK, and recruitment had to pause during the COVID pandemic, although the investigators believed the pandemic did not materially change the main findings, it could have as for many people, self-isolating reduced infective exacerbations. These do not invalidate the trial, but they remind us that a trial is never the whole story.
Why Dr Ricardo José would still recommend it for selected patients
Dr Ricardo Jose’s approach to bronchiectasis care strongly emphasises airway clearance, thick mucus management, and individualised treatment. In that context, it is reasonable to continue recommending nebulised hypertonic saline for a carefully selected patient whose main problem is tenacious sputum, difficult clearance, and persistent mucus impaction despite good physiotherapy technique.
That does not mean ignoring the RCT. It means using it properly. The negative trial suggests hypertonic saline should not be prescribed routinely for everyone with bronchiectasis just because they have the diagnosis. But it does not prove that no one benefits.
In practice, doctors often treat patterns, not just averages. If a patient clearly coughs up more sputum, feels less chest congestion, has fewer plugs on imaging, or finds daily airway clearance much easier on hypertonic saline, that personal response still matters.
This is very much in line with guideline-style thinking. British guidance has advised considering a trial of mucoactive treatment in patients who have difficulty with sputum expectoration, and NHS guidance still describe hypertonic saline as an option when airway clearance alone is not enough.
Who is most likely to be the “right” patient?
A patient-friendly way to think about it is this: nebulised hypertonic saline may make more sense when the problem is clearly mechanical mucus blockage rather than simply frequent infections alone. The sort of patient Dr José would still think about is someone with:
– chronic thick, sticky sputum;
– mucus that remains hard to shift even after proper teaching and optimisation of airway clearance;
– evidence of mucus impaction on CT or other imaging;
– ongoing chest congestion where the goal is to move secretions better, not just to chase a trial endpoint.
It should still be used carefully. Hypertonic saline can cause cough, throat irritation, chest tightness, or shortness of breath, so Dr José recommends a supervised first dose or airway reactivity check, and sometimes bronchodilator pre-treatment.

Conclusion
The CLEAR trial was negative, and that is important. The trial shows that nebulised hypertonic saline is not a universal answer for all adults with bronchiectasis, and clinicians should not prescribe it automatically in the hope that it will reduce flare-ups across the board.
But a negative average result does not erase real-world benefit in the right patient. The CLEAR study still leaves open the possibility that people with the thickest, hardest-to-clear sputum may respond differently, because the researchers did not specifically include that group or design the trial to detect benefits in subgroups.
Dr Ricardo José still recommends optimising airway clearance first. He then considers nebulised hypertonic saline for patients with viscous mucus, difficulty clearing secretions, and mucus impaction on imaging. In these patients, the treatment can still make a meaningful difference to symptoms and day-to-day lung clearance. This may happen even though the trial did not show benefit for its main headline outcome.
Frequently asked questions
1. Does a negative RCT mean nebulised hypertonic saline does not work?
No. It means the treatment did not show a statistically significant benefit for the average patient in that trial on the trial’s main outcome. It does not prove that selected patients cannot benefit.
2. What did the CLEAR trial actually show?
It showed that, over 52 weeks, adding 6% hypertonic saline did not significantly reduce exacerbations compared with no hypertonic saline in the overall study population.
3. Why might some doctors still use nebulised hypertonic saline?
Because some patients mainly struggle with thick, sticky mucus and mucus plugging. In that situation, a treatment that makes mucus less sticky may still improve daily clearance, even if it does not clearly reduce annual flare-ups in a broad trial population.
4. Who may be most likely to benefit?
Specialists are most likely to consider an individual trial of treatment in patients who have viscous sputum, difficulty clearing mucus despite well-taught airway clearance, and mucus impaction on imaging.
5. Are there side effects?
Yes. Some people get cough, throat irritation, chest tightness, wheeze, or shortness of breath. That is why clinicians often supervise the first dose and ask some patients to use a bronchodilator beforehand.
GET IN TOUCH
Schedule a Visit with Dr Jose
For an assessment of your diagnosis and treatment.
Disclaimer: The information provided in this article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment, and is not an advertisement for medical products. Always seek the advice of your healthcare provider with any questions you may have regarding a medical condition or treatment. Your healthcare professional can assess your individual circumstances. Consultation does not guarantee suitability for any specific treatment; all clinical decisions follow an individual assessment and shared decision-making
