A lung function test may be recommended if you have symptoms that suggest your lungs or airways are not working as well as they should. These symptoms can include shortness of breath, wheezing, a persistent cough, chest tightness, reduced exercise tolerance, or feeling unusually breathless during everyday activities.
Lung function testing is commonly used to help assess conditions such as asthma, chronic obstructive pulmonary disease, emphysema, pulmonary fibrosis, and other respiratory conditions. It may also be used to monitor an existing lung condition, check how well treatment is working, or assess breathing before certain types of surgery.
You may also be advised to have a lung function test if you smoke or used to smoke, have workplace exposure to dust or chemicals, have a family history of lung disease, or have ongoing breathing symptoms after a chest infection.
Tests carried out in the lung function laboratory include:

Spirometry allows the determination of airflow limitation in the lungs. The individual will be asked to wear a clip on their nose that prevents air from escaping from the nose. Following a deep breath they are asked to blow out as quickly and as forcibly as they can into a mouth piece.
In addition to identifying airflow limitation in your airways spirometry allows determination of obstructive and restrictive lung disease. For example, to differentiate between asthma and COPD, or interstitial lung disease, or chest wall restriction.
Sometimes a bronchodilator such as salbutamol is administered and the spirometry test repeated 15 min later. This will allow to determine if their is significant dilatation of the airways. Significant bronchodilator reversibility as seen in asthma is an increase in forced expiratory volume in 1 second of 12% or more or more than 200 mL.
Body plethysmography is a test used to determine lung volumes. For example, it can determine your total lung capacity (ie. how much total amount of air in the lungs at the end of full inspiration) and the residual volume (ie. the total amount of air in the lungs at the end of full expiration). People with restrictive lung disease have reduced lung volumes and those with obstructive lung disease may have a increased residual volume because narrow airways cause air to be trapped in the lungs as it isn’t completely exhaled.
This tests is also known as transfer factor or diffusing capacity. It is a measure of how well the lungs exchange gases between themselves and the blood. To do this test a mixture containing a small amount of helium and carbon monoxide is inhaled through a deep breathe. After a breath hold of 8 to 10 seconds the air from the lungs is slowly exhaled into the machine for a reading. To get an accurate representation the value obtained needs to be corrected for the lung volume and the haemoglobin in blood as these two parameters affect the transfer factor value. A low transfer factor indicates impaired gas exchange.
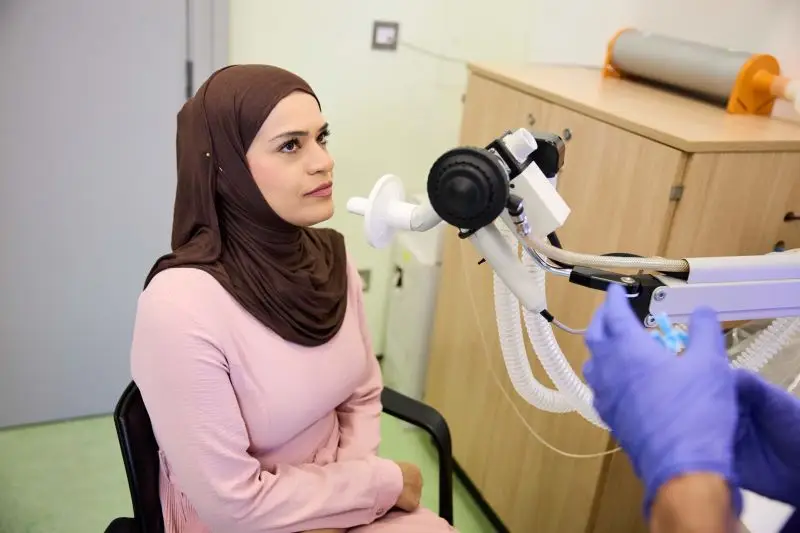
Respiratory muscle tests are useful to determine if the breathing problem is due to weak respiratory muscles. These tests include:
Mouth pressures
After breathing our air from the lungs as long as possible the person is asked to suck hard on a mouthpiece for 1 second to measure the maximal inspiratory pressure. Then after taking a deep breath in the person exhales forcibly against a closed off mouthpiece to determine the maximal expiratory pressure.
Sniff pressures
A small probe is inserted into one nostril and measures the inspiratory and expiratory pressures when the person sniffs.
Lying and sitting / standing vital capacity
Spirometry is done lying down in the supine position and then again in a sitting or standing position. A significant reducation in the supine VC may suggest respiratory muscle and diaphragmatic weakness.
Inflammation in the lungs can produce nitric oxide and high levels of NO (>40 ppb) may suggest asthma. However not all types of asthma will produce a high level of NO. This test involves taking in a deep breath and then slowly exhaling at a constant rate into the machine that takes the reading.
This test mimics the conditions in a pressurised cabin at altitude. Although an airplane may be flying at higher altitude the cabin is pressurised to 5000 – 8000 feet where the oxygen concentration in air is reduced from 21% to 15%. For people with healthy lungs and oxygen saturations >94% this isn’t a problem. But for people with signifcant respiratory disease and oxygen saturations >95% there oxygen saturations may drop significantly during the flight leading to respiratory distress.
To do the test the person sits in a cabin breathing air with 15% oxygen and using a pulse oximeter the oxygen saturation is monitored and is used to determine if the person needs oxygen during a flight, and if they do, how much oxygen per minute they will need.
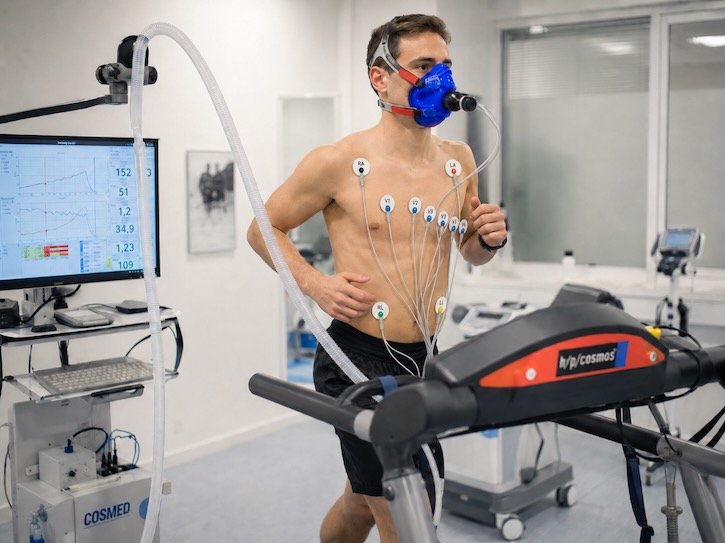
Cardiopulmonary exercise testing, also known as CPET or CPEX, is a specialised test that provides information on how the heart, lungs and muscles are working together during exercise. It can therefore help determine if breathlessness is caused by a problem with the heart or lungs, a combination of the two, breathing pattern disorder or lack of fitness. It is also very useful to determine fitness before major surgery.
For the test the person will exercise on an upright stationary bicycle or treadmill. They will breathe through a mouthpiece and recordings are taken from the breath, from heart monitors (continuous electrocardiogram and regular blood pressure). Capillary or arterial blood gases are also taken to measure blood oxygen, carbon dioxide and lactate levels.
Your lung function centre will tell you how to prepare for your lung function test, as the advice can vary depending on the type of test you are having and whether you use inhalers or other respiratory medicines.
Before your appointment, you may be asked to avoid smoking, vaping, alcohol, strenuous exercise, or eating a large meal for a set period of time. You may also be advised to wear loose, comfortable clothing so that you can breathe fully during the test. Some people are asked to stop using certain inhalers before spirometry.
Bring a list of your current medicines, including inhalers, and let the clinician know if you have recently had a chest infection, surgery, chest pain, or any change in your breathing symptoms.
Some lung function tests require you to avoid certain inhalers beforehand, because inhalers that open the airways can affect the test results. This is especially important if the test is being done to assess your baseline breathing, confirm a diagnosis, or check whether your breathing improves after a reliever inhaler.
You should only stop or delay inhalers if you have been specifically advised to do so by your healthcare team. If your breathing becomes worse, or you need your reliever inhaler, use it as prescribed and tell the clinician when you arrive for your appointment.
As general guidance, you may be asked to avoid:
| Type of inhaler | Examples | Typical time to avoid before testing |
|---|---|---|
| Short-acting reliever inhalers | Salbutamol, Ventolin, terbutaline, Bricanyl | Around 4–6 hours |
| Short-acting muscarinic antagonist inhalers | Ipratropium | Around 12 hours |
| Long-acting bronchodilator inhalers | Formoterol, salmeterol-containing inhalers | Around 12–24 hours, depending on the medicine |
| Long-acting muscarinic antagonist inhalers | Tiotropium, umeclidinium, glycopyrronium-containing inhalers | Often 24–36 hours |
| Ultra-long-acting or once-daily inhalers | Some once-daily LABA/LAMA or combination inhalers | May need longer withholding, depending on the inhaler |
Please bring all your inhalers, spacers, and a list of your medicines to the appointment. If you have used an inhaler within the advised withholding period, the test may still be possible, but the clinician will need to record what you took and when.
To help make the result as accurate as possible, you may be asked to avoid the following before your FeNO test:
| What to avoid | How long before the test |
|---|---|
| Smoking or vaping | At least 1 hour |
| Strenuous exercise | At least 1 hour |
| Hot drinks | At least 1 hour |
| Caffeine, including tea, coffee, cola, and energy drinks | At least 1 hour |
| Alcohol | At least 1 hour |
| Nitrate-rich foods, such as beetroot, spinach, lettuce, celery, leek, cabbage, and other green leafy vegetables | At least 3 hours |
You can usually continue your regular inhalers and medicines before a FeNO test unless your healthcare team tells you otherwise. Let the clinician know if you have recently had a chest infection, used your inhaler shortly before the test, smoked, exercised, or eaten nitrate-rich foods before your appointment.
A lung function test checks how well your lungs are working. It can measure how much air you can breathe in and out, how quickly you can blow air out, and in some cases how well oxygen passes from your lungs into your blood.
Spirometry is one of the most common types of lung function test. It measures airflow and is often used to help assess symptoms such as breathlessness, wheezing, coughing, or suspected asthma or COPD.
The length of the appointment depends on which tests you need. Simple spirometry may only take a short time, while full lung function testing can take longer if several measurements are required.
No. Lung function tests are not usually painful. You may feel temporarily breathless, lightheaded, or tired because the test involves deep breathing and forceful blowing.
Lung function tests can provide important information that helps clinicians assess asthma, COPD, and other respiratory conditions. However, results are usually interpreted alongside your symptoms, medical history, examination, and sometimes other investigations.
You may be asked to avoid certain inhalers before the test, but this depends on the reason for the test and the type of inhaler you use. Follow the instructions given by your healthcare team and do not stop prescribed medicine unless you have been told to.
Wear loose, comfortable clothing that does not restrict your chest or abdomen. This helps you breathe in and out fully during the test.
Your lung function test results will be discussed at your follow up consultation. You will then copies of all your lung function test results.