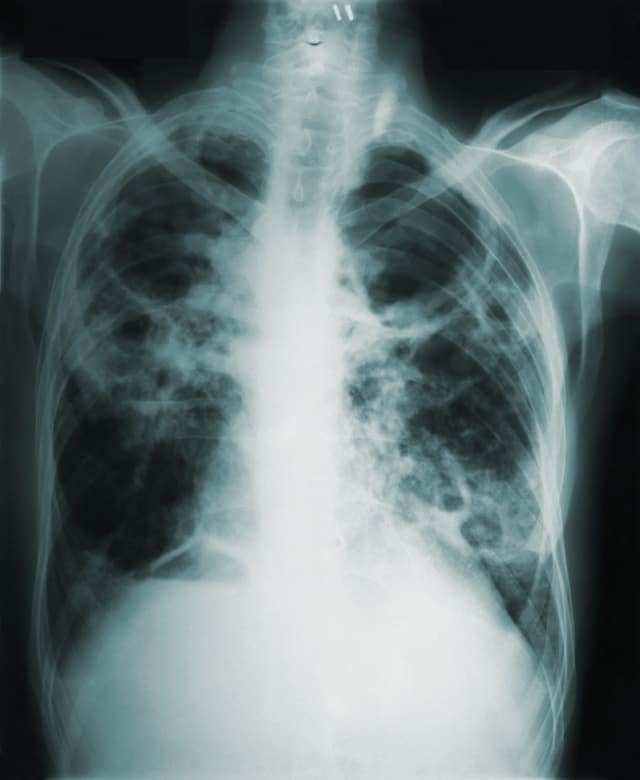
Introduction to Tuberculosis
Tuberculosis, often referred to as TB, is an infectious disease caused by the bacterium Mycobacterium tuberculosis. This ancient and notorious disease has plagued humanity for centuries, leaving behind a trail of suffering and death. Despite advancements in medicine and healthcare, tuberculosis remains a significant global health concern, particularly in resource-limited regions.
Epidemiology of Tuberculosis
Understanding the epidemiology of tuberculosis is vital in comprehending the disease’s scope, distribution, and impact on public health. Tuberculosis continues to be a major global health concern, affecting people of all ages and socioeconomic backgrounds. In this section, we delve into the key epidemiological aspects of TB, providing insights into its prevalence, risk factors, and regional disparities.
Global Burden of Tuberculosis
Tuberculosis has a significant global burden, with millions of new cases reported each year. According to the World Health Organization (WHO), approximately 10 million people developed active TB disease in the latest reported year. The disease’s impact extends beyond morbidity and mortality, as it also poses economic challenges to communities and nations.
Regional Variations
Tuberculosis exhibits regional variations in its prevalence and incidence rates. High-burden countries with a high number of TB cases include India, China, Indonesia, the Philippines, Pakistan, Nigeria, and South Africa. These regions face challenges related to population density, poverty, limited access to healthcare, and other risk factors contributing to TB transmission.
Socioeconomic Factors
Tuberculosis disproportionately affects marginalized and vulnerable populations. Factors such as poverty, malnutrition, overcrowded living conditions, and inadequate access to healthcare facilities increase the risk of contracting TB. Additionally, populations with weakened immune systems, such as those living with HIV/AIDS, are more susceptible to TB infection and progression to active disease.
Drug-Resistant Tuberculosis
The emergence of drug-resistant tuberculosis poses a serious threat to global TB control efforts. Multidrug-resistant tuberculosis (MDR-TB) and extensively drug-resistant tuberculosis (XDR-TB) are challenging to treat and require specialized medications. Inappropriate use of antibiotics and treatment non-adherence contribute to the development of drug-resistant TB strains.
Tuberculosis in High-Risk Groups
Certain population groups are at higher risk of TB infection and disease. These groups include healthcare workers, prisoners, migrants, refugees, and individuals living in high-density urban areas or congregate settings. Targeted interventions and screening programs in these populations are essential to prevent TB transmission.
Latent TB Infection
In addition to active TB disease, there are vast numbers of individuals with latent TB infection (LTBI). LTBI occurs when a person carries the TB bacteria but does not have active symptoms or transmit the disease to others. People with LTBI are at risk of developing active TB in the future, particularly if their immune system becomes compromised.
Transmission and Risk Factors
Tuberculosis primarily spreads through the air when an infected individual coughs or sneezes, releasing tiny droplets containing the tuberculosis bacteria. People who are in close contact with infected individuals are at higher risk of contracting the disease. Moreover, certain factors such as weakened immune systems, malnutrition, and crowded living conditions increase susceptibility to tuberculosis.
Signs and Symptoms of Tuberculosis
The symptoms of tuberculosis can be subtle and develop gradually, often resembling those of other respiratory illnesses. Common signs include persistent cough, fever, night sweats, and unexplained weight loss. Tuberculosis can affect various organs, leading to a range of additional symptoms and complications.
Diagnosis and Screening
Detecting tuberculosis requires a combination of diagnostic tests. The tuberculin skin test (TST) and Interferon-Gamma Release Assays (IGRAs) help identify latent TB infection. Imaging methods like chest X-rays aid in identifying active TB disease. Sputum tests and nucleic acid amplification tests (NAATs) are vital for confirming the presence of M. tuberculosis.
Preventive Measures
Preventing tuberculosis involves several approaches, including the Bacille Calmette-Guérin (BCG) vaccine, which offers partial protection against severe forms of the disease. For individuals with latent TB infection, preventive treatment reduces the risk of progressing to active TB disease. Infection control measures are essential in healthcare settings and communities with high TB prevalence.
Tuberculosis Treatment and Medications
The treatment of tuberculosis (TB) involves a combination of antimicrobial drugs that target the causative agent, Mycobacterium tuberculosis. The choice of medications, treatment duration, and regimens depend on the type of TB (latent or active) and the presence of drug resistance. The standard TB treatment aims to achieve cure and prevent relapse while minimizing the risk of drug resistance. In recent years, advancements in research have led to newer treatment regimens that seek to reduce the duration of treatment, improving patient adherence and outcomes.
First-Line Drugs for Tuberculosis
The first-line drugs used in the treatment of TB include:
- Isoniazid: Isoniazid is a key drug for TB treatment and is highly effective against actively dividing TB bacteria. It is also used as a prophylactic drug for individuals with latent TB infection.
- Rifampin: Rifampin is another crucial drug in TB treatment. It works by inhibiting the synthesis of RNA in TB bacteria, effectively killing them.
- Pyrazinamide: Pyrazinamide is particularly effective against TB bacteria residing in acidic environments, such as inside macrophages.
- Ethambutol: Ethambutol is active against TB bacteria and helps prevent the development of drug resistance when used in combination with other first-line drugs.
Standard TB Treatment Regimen
The standard treatment regimen for drug-sensitive TB typically lasts for six months and involves a two-month intensive phase, followed by a four-month continuation phase. The intensive phase consists of four drugs: INH, RIF, PZA, and EMB. After the intensive phase, the continuation phase includes INH and RIF.
Directly Observed Therapy (DOT)
Directly Observed Therapy (DOT) is a strategy recommended by the World Health Organization (WHO) to enhance treatment adherence and reduce the risk of drug resistance. In DOT, a healthcare provider or designated individual directly observes the patient taking their medication.
Multidrug-Resistant Tuberculosis (MDR-TB)
In cases of drug-resistant TB, treatment becomes more challenging. Multidrug-resistant tuberculosis (MDR-TB) is resistant to at least Isoniazid and Rifampicin, the two most potent first-line drugs. Treating MDR-TB requires a longer duration (usually 9-20 months) and a combination of second-line drugs, which are less effective and may have more significant side effects.
Newer Treatment Regimens
To tackle the difficulties of MDR-TB treatment and shorten the overall duration of TB treatment, newer treatment regimens have been developed. These regimens are collectively known as “Shorter Treatment Regimens” and offer significant advantages:
- 9-Month Regimen: This regimen for drug-sensitive TB shortens the treatment duration from six to nine months, making it more manageable for patients to complete the course.
- “All-Oral” Regimens: Some new treatment regimens consist entirely of oral medications, eliminating the need for injectable drugs that can cause discomfort and complications.
- Bedaquiline: Bedaquiline is a novel drug that has shown promising results in treating MDR-TB. It is a part of some newer regimens and significantly improves treatment outcomes.
- Delamanid: Delamanid is another drug approved for MDR-TB treatment and contributes to more effective and shorter treatment regimens.
Importance of Completing the Full Course
Regardless of the treatment regimen, completing the full course of TB medication is crucial. Partial or inadequate treatment can lead to treatment failure, drug resistance, and relapse. Patients must strictly adhere to their prescribed medication schedule and promptly report any side effects to their healthcare providers.
Drug Interactions and Side Effects
While tuberculosis (TB) treatment is highly effective, it can be associated with side effects that may impact patients’ well-being and treatment adherence. It is essential for healthcare providers and patients to be aware of these side effects and take appropriate measures to manage them effectively. Regular monitoring during treatment is crucial to ensure patient safety and successful outcomes.
Common Side Effects of TB Medications:
- Gastrointestinal Disturbances: Nausea, vomiting, and stomach upset are common side effects of TB drugs, especially during the initial phase of treatment. Taking medications with food or milk can help reduce these symptoms.
- Hepatotoxicity: Some TB drugs, particularly isoniazid and rifampin, can affect the liver. Patients may experience elevated liver enzyme levels, which can be monitored through blood tests. Prompt reporting of any signs of jaundice or dark urine is crucial.
- Peripheral Neuropathy: Isoniazid can cause nerve damage, leading to tingling or numbness in the hands and feet. Taking vitamin B6 (pyridoxine) supplements can help prevent or alleviate this side effect.
- Visual Disturbances: Ethambutol may lead to visual changes or blurred vision. Regular eye examinations are essential during treatment to detect any ocular issues.
- Rash and Allergic Reactions: Skin rashes and allergic reactions can occur as a response to TB medications. Patients should inform their healthcare providers immediately if they experience any skin changes or allergic symptoms.
- Joint Pain: Some individuals may experience joint pain or arthralgia during TB treatment. Over-the-counter pain relievers can help manage this discomfort.
Managing Side Effects:
- Supportive Care: Adequate hydration, a balanced diet, and regular exercise can help support the body during TB treatment and alleviate some side effects.
- Patient Education: Patients should be educated about potential side effects before starting treatment. Knowing what to expect and how to manage them can improve treatment adherence.
- Drug Interaction Management: Informing healthcare providers about all medications and supplements being taken can help avoid harmful drug interactions.
- Vitamin Supplementation: Taking vitamin B6 supplements can help prevent peripheral neuropathy caused by isoniazid.
- Medication Adjustment: In some cases, healthcare providers may adjust the dose or switch medications to minimize side effects while maintaining treatment efficacy.
Monitoring During Treatment:
Regular monitoring during TB treatment is essential to assess treatment progress and identify any potential complications. Monitoring includes:
- Clinical Evaluation: Regular check-ups with healthcare providers to assess treatment response and monitor for any new symptoms or side effects.
- Laboratory Tests: Periodic blood tests to monitor liver function, kidney function, and other important parameters.
- Eye Examinations: Ophthalmologic assessments to detect any visual disturbances related to ethambutol.
- Adherence Monitoring: Ensuring patients take their medications as prescribed is vital for successful treatment outcomes.
Public Health Initiatives
Tuberculosis control is a global effort spearheaded by organizations like the World Health Organization (WHO). Collaborative efforts aim to improve diagnostics, treatment access, and raise awareness of tuberculosis as a public health priority. However, challenges like drug resistance and funding limitations persist.
Social Stigma and Tuberculosis
Stigma surrounding tuberculosis can hinder prevention efforts and patient care. Overcoming stigma involves educating communities, fostering empathy, and supporting those affected by the disease. By breaking down barriers, we can create a more inclusive and compassionate approach to tuberculosis management.
TB and HIV Co-infection
Tuberculosis and HIV/AIDS often coexist, creating a complex challenge for healthcare providers. The weakened immune system in HIV-positive individuals increases the risk of developing active TB disease. Integrated strategies that address both infections are essential for improved outcomes.
Nutrition and Tuberculosis
Nutrition plays a crucial role in tuberculosis treatment and recovery. Adequate nutrient intake helps support the immune system and improves treatment response. Providing nutritional support to TB patients is vital, especially in regions with high malnutrition rates.
Tuberculosis in the Elderly
Elderly individuals may face additional challenges during tuberculosis treatment due to age-related factors. Addressing these concerns and providing tailored care is crucial to ensuring positive outcomes and maintaining overall well-being in older TB patients.
Conclusion
Tuberculosis remains a formidable global health challenge, but concerted efforts in research, prevention, and treatment offer hope for a tuberculosis-free future. By understanding the disease, raising awareness, and promoting compassionate care, we can work together to eradicate tuberculosis and improve the lives of millions worldwide.
GET IN TOUCH
Schedule a Visit with Dr Ricardo Jose
Disclaimer: The information provided in this article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your healthcare provider with any questions you may have regarding a medical condition or treatment
