We live in a world teeming with invisible life forms. One such organism that has emerged as a major concern in recent years is Pseudomonas Aeruginosa. You might not have heard of it, or you might have come across this term but haven’t quite understood what it signifies. It’s not as familiar as common germs like Escherichia coli or Staphylococcus aureus, but it’s no less important.
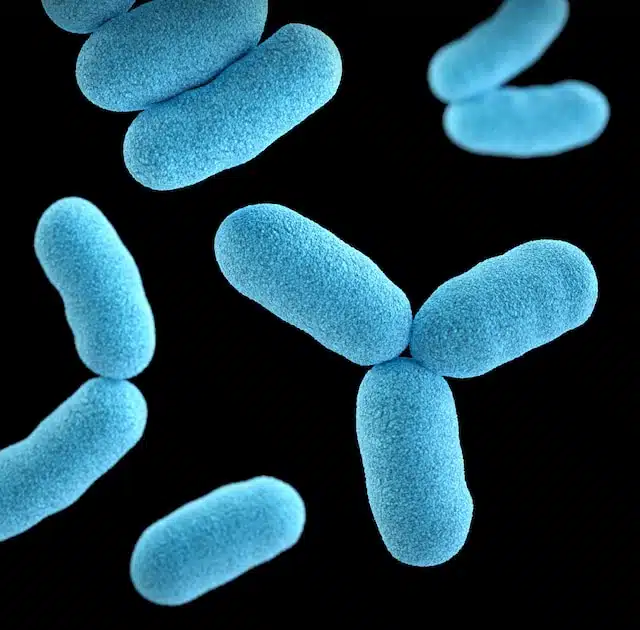
What is Pseudomonas Aeruginosa?
Pseudomonas Aeruginosa is a common bacterium, one of many Pseudomonas species. It’s versatile and can adapt to a variety of environments. As an opportunistic pathogen, it primarily affects individuals with compromised immune systems or with structural lung fisease but can also infect healthy people, given the right conditions.
Where is Pseudomonas Aeruginosa Found?
Pseudomonas Aeruginosa is incredibly resilient. It thrives in many environments: soil, water, plants and even most man-made surfaces. Surprisingly, it can even survive in disinfectant solutions, which are typically designed to kill bacteria.
The Impact of Pseudomonas Aeruginosa on Human Health
This bacterium can cause a variety of infections, from minor skin infections to life-threatening systemic infections. However, its impact on lung function is most notable. It’s implicated in several lung-related diseases, including pneumonia, hospital-acquired pneumonia and, especially, in colonising the airways of people bronchiectasis.
Pseudomonas Aeruginosa pneumonia often strikes patients in hospital settings, particularly those with weakened immune systems. It’s notorious for causing ‘hospital-acquired pneumonia’, a leading cause of death in intensive care units.
Bronchiectasis patients face a particularly high risk from Pseudomonas Aeruginosa. In this condition, the airways in the lungs become damaged and widened, making it harder for them to clear mucus. This creates a perfect environment for Pseudomonas Aeruginosa to thrive, leading to repeated infections that further damage the lungs.
The Challenge of Multi-Drug Resistant Pseudomonas Aeruginosa
One of the biggest challenges with Pseudomonas Aeruginosa is its growing resistance to multiple drugs. This makes treatment more complex and often less successful. The rise in multi-drug resistance is a critical concern worldwide and presents a considerable obstacle to controlling infections effectively.
Treating Pseudomonas Aeruginosa Infections
Several antibiotics are effective against Pseudomonas Aeruginosa, including piperacillin/tazobactam, ceftazidime, and tobramycin. These can be given intravenously or even inhaled using a nebuliser. However, oral antibiotic options are limited and somewhat restricted to ciprofloxacin.
A nebuliser is a device that turns liquid medicine into a fine mist, which can then be inhaled deep into the lungs. This is particularly useful in treating lung infections caused by Pseudomonas Aeruginosa, as it delivers the drug directly to the infection site.
However, because of the rise of multi-drug resistant strains, treatment options are becoming increasingly limited. Often, combinations of antibiotics are used in an attempt to overcome resistance. Research is ongoing looking at the development on novel antibiotics, anti-pseudomonal antibodies and phage therapy.
Key messages
Pseudomonas Aeruginosa is a bacterium that presents a real and ongoing threat to human health, especially in hospital environments. It’s especially dangerous for people with lung diseases like bronchiectasis, as it can lead to repeated, damaging lung infections.
While antibiotics remain our primary tool against this pathogen, the increasing prevalence of multi-drug resistant strains is worrying. As a society, we need to continue investing in research to develop new treatments and combat this growing threat.
Understanding Pseudomonas Aeruginosa is not just for health professionals; it’s important for everyone. As this invisible enemy becomes more prevalent, staying informed is a crucial step in staying safe.
GET IN TOUCH
Schedule a Visit
Disclaimer: The information provided in this article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your healthcare provider with any questions you may have regarding a medical condition or treatment.
